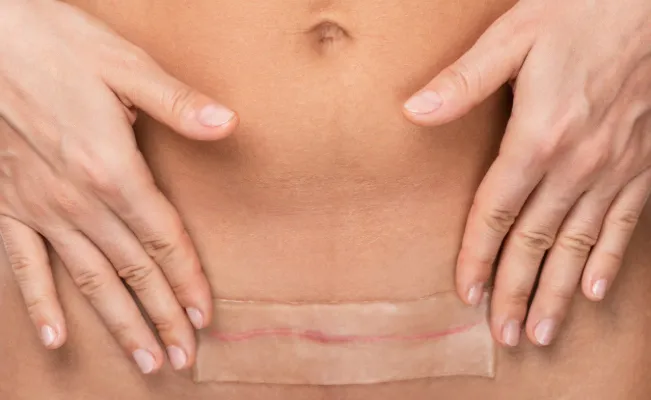
Your cesarean incision left you with more than a scar; it's a story of strength. Here's what you need to know about the different types.
If you're recovering from a C-section (or preparing for one) you've probably heard terms like "bikini cut" or "horizontal incision" tossed around. But what do these different C-section incision types actually mean for your scar, your recovery, and even future pregnancies?
Let's break it down together. This guide walks you through the types of cuts doctors make (yes, there's more than one layer), what your scar might look like as it heals, and something many moms don't realize: how a C-section birth affects your baby's health too. You deserve clear answers, so here they are.
Two Cuts, Two Stories: Cesarean Section Incision Types
Here's something that surprises many moms: during your C-section, your doctor actually makes two separate incisions. There’s one on your tummy (the abdominal incision) and a separate one on your uterus where your baby is nestled (the uterine incision).1
- Abdominal incision or laparatomy (the outer scar): This is the cut you can see and feel on your belly. It determines what your scar looks like and how visible it'll be under clothing.2
- Uterine incision or hysterotomy (the inner cut): This is the cut on your uterus itself, hidden inside. You won't see it, but it's crucial for future pregnancies and VBAC (vaginal birth after cesarean) eligibility. Your doctor chooses this based on your baby's position, placenta location, and other medical factors.2
Your external scar doesn't automatically tell you what type of uterine incision you have. They're chosen independently based on what's safest for you and baby.
| Incision Types | What It Is | Common Types |
|---|---|---|
| Abdominal | The visible cut on your belly that becomes your scar | Horizontal (bikini cut/low transverse), Vertical (midline) |
| Uterine | The cut made on your uterus to deliver baby | Low transverse, Low vertical, Classical (high vertical) |
Your Abdominal Cut: The Scar You'll See and Care For
This is the incision you'll actually see: the one that becomes your C-section scar.1 It's what you'll clean, moisturize, and watch heal over the coming months. Most moms get one of two types.3
Horizontal or Low Transverse (Bikini Cut)
This is a side-to-side cut just above your pubic bone, following your skin's natural crease. It's usually 4–6 inches long and sits low enough to be hidden by underwear or swimwear. This is the most common choice because it heals well, has a lower infection risk, and leaves a less noticeable scar.4
What it looks like: a thin horizontal line that fades from pink or red to pale over time.
Vertical or Midline
This is an up-and-down cut from below your belly button toward your pubic area, typically 5–7 inches long and more visible. It's less common today but sometimes medically necessary.4
What it looks like: a vertical line down your lower belly that may be slightly more raised than a horizontal scar.
When Is a Vertical Cut Used?
Your doctor might choose a vertical incision in specific situations, and it's always about safety, not preference:
- Emergency deliveries where speed is critical
- Very premature babies who need gentler, faster delivery
- Certain baby positions (like transverse/sideways)
- Previous abdominal surgeries or scar tissue
- Some placenta complications
If you have a vertical scar, it doesn't mean something went wrong. It means your doctor prioritized getting your baby out safely.5
The Cut You Can't See: Understanding Uterine Incision
While your abdominal scar is visible, there's another incision that matters just as much—the cut made on your uterus to deliver your baby. Here's the thing: your uterine incision type doesn't always match your skin incision.6
You could have a horizontal bikini-cut scar on your belly but a different type of cut on your uterus. This “hidden” incision is especially important if you're considering VBAC (vaginal birth after cesarean) in the future.
- Low transverse (horizontal): A side-to-side cut in the lower, thinner part of your uterus. This is by far the most common (about 95% of cesareans) and the safest for future pregnancies. It heals strongest and has the lowest risk of uterine rupture, making it VBAC-friendly.6
- Low vertical: An up-and-down cut in the lower uterus. Less common but used in certain situations. VBAC may still be possible, though it carries slightly higher risk than low transverse. Your doctor will evaluate your specific case.7
- Classical (high vertical): A vertical cut in the upper, thicker part of your uterus. Rarely used today—only in urgent situations or specific medical circumstances. This type typically rules out VBAC due to higher rupture risk in future labor.7
| Incision Types | Location & Description | Future Pregnancy/VBAC |
|---|---|---|
| Low Transverse | Horizontal cut on the lower, thinnest part of the uterus. | Safest: Allows for possible VBAC (aka Trial of Labor after Cesarean or TOLAC). |
| Low Vertical | Vertical cut only in the lower part of the uterus. | Higher Risk: VBAC may still be considered, but risk is increased. |
| High Vertical (Classical) | Vertical cut extending into the muscular upper part of the uterus. | Highest Risk: VBAC is generally not recommended. |
Two Recoveries, One Journey: Your CS Incision Types and Your Baby's Start
As you focus on healing your incision (keeping it clean, watching for infection signs, and giving your body time to recover), there's another kind of recovery happening that's easy to miss: your CS-born child's gut development.
Did you know that babies born by C-section miss out on the beneficial bacteria they would normally pick up passing through the birth canal? This difference (often called dysbiosis) affects their early gut microbiome: the community of bacteria that supports digestion, immunity, and even brain development.8
This difference in early gut health matters because research shows it can potentially impact a child's immunity, making them more prone to respiratory and metabolic issues such as asthma and type 1 diabetes as they grow older.9
Why the gut-brain connection matters: Your child's gut and brain are in constant communication through what scientists call the gut-brain axis.10 When gut bacteria are out of balance early in life, it can potentially affect how the brain develops, influencing everything from learning and behavior to emotional regulation as your child grows.11
What this means for CS babies:9,10,11
- Lower levels of helpful or “good bacteria” like Bifidobacteria in early months
- Babies at risk of dysbiosis (bacterial imbalance) that can persist beyond preschool age
- Potential links to digestive issues, allergies, and immune differences as they grow
- Early gut microbiome imbalance which may affect brain development
Nutrition That Supports Your CS Kid’s Gut and Brain Health
Here's the encouraging part: your child's microbiome and brain development can be supported with targeted nutrition. Research shows that supplementation with specific nutrients can help promote a healthier gut microbiome in CS-born kids.12
| Nutrient | How It Helps CS-Born Kids |
|---|---|
| Prebiotics | Nourish beneficial gut bacteria, helping rebalance the microbiome after CS birth. |
| DHA | Supports brain structure and cognitive development; works synergistically with healthy gut bacteria. |
| MFGM (Milk Fat Globule Membrane) | Found naturally in breast milk; supports gut barrier function and brain development pathways. |
Just as your scar heals with proper care, your child's microbiome can be nurtured with Enfagrow CS-Biome 3+. It is specially designed for CS-born kids with its unique C-Biome Blend—the only milk formulated with MFGM + the highest DHA levels (among formula milks), for brain development and an Exclusive Immune Blend with Prebiotics to help support gut microbiome. By addressing dysbiosis early, Enfagrow CS-Biome 3+ helps provide the STRONGER PROTECTION your child needs for their brain, immunity, and gut, ensuring they have an A+ start in life. (vs. both regular cow’s milk and formula without MFGM, all with proper nutrition and stimulation, supplementation was done during the first year of life)

Your C-Section Incision Type: Both of You Deserve the Best Care
Understanding the different C-section incision types helps you know what to expect as you heal. Just as you begin your recovery journey by tending to your scar inside and out, your CS-born child needs targeted support for their unique start, especially when it comes to building a healthy gut microbiome.
That's where #Enfagrow CS-Biome 3+ comes in — the only milk with MFGM and the highest DHA levels(among formula milks), specially designed with C-Biome Blend (Exclusive Immune Blend + Prebiotics + MFGM & DHA) to help CS-born kids’ STRONGER PROTECTION for brain, immunity, and gut. Because every CS baby deserves an exceptional start. (vs. both regular cow’s milk and formula without MFGM, all with proper nutrition and stimulation, supplementation was done during the first year of life)
Frequently Asked Questions
What are the two types of incisions used for a C-section?
A C-section actually involves two separate incisions—an abdominal (skin) incision you can see, and a uterine incision on your uterus that's hidden inside. The most common skin incisions are horizontal (bikini cut) or vertical (midline), while uterine incisions can be low transverse, low vertical, or classical.1
What is the most common incision for a C-section?
The horizontal low transverse incision (bikini cut) is most common because it heals faster and is easily hidden by underwear.4
How long does a C-section incision take to heal?
Your incision typically closes within 2–6 weeks, but complete scar healing and maturation takes 3-12 months as the tissue strengthens and the scar fades.
References
- Sung, S., Mikes, B. A., Martingano, D. J., & Mahdy, H. (2024). Cesarean Delivery (PMID 31536313). National Library of Medicine, National Center for Biotechnology Information. https://www.ncbi.nlm.nih.gov/books/NBK546707/https://www.ncbi.nlm.nih.g…
- Mayo Clinic Staff. (2025, August 29). C-section. Mayo Clinic. https://www.mayoclinic.org/tests-procedures/c-section/about/pac-2039365…
- Mayo Clinic Staff. (n.d.). Abdominal incisions used during C-section. Mayo Clinic. https://www.mayoclinic.org/tests-procedures/c-section/multimedia/abdomi…
- Higuera, V. (2020, January 28). C-section scars: Types of incisions, healing, and minimizing scars. Healthline. https://www.healthline.com/health/pregnancy/c-section-scarhttps://www.h…
- Kan, A. (2020). Classical cesarean section. The Surgery Journal, 06(S 02). https://doi.org/10.1055/s-0039-3402072https://doi.org/10.1055/s-0039-34…
- Jacobson, J. D., & Linda, L. (2024, October 15). C-section – series-procedure, part 3. MedlinePlus. https://medlineplus.gov/ency/presentations/100191_5.htmhttps://medlinep…
- Glover, A. (2025, August). Deciding between a VBAC and a repeat cesarean: 7 questions to ask. ACOG. https://www.acog.org/womens-health/experts-and-stories/the-latest/decid…
- Salas Garcia, M. C., Yee, A. L., Gilbert, J. A., & Dsouza, M. (2018). Dysbiosis in children born by caesarean section. Annals of Nutrition and Metabolism, 73(Suppl. 3), 24–32. https://doi.org/10.1159/000492168https://doi.org/10.1159/000492168
- Zhang, C., Li, L., Jin, B., Xu, X., Zuo, X., Li, Y., & Li, Z. (2021). The effects of delivery mode on the gut microbiota and health: State of art. Frontiers in Microbiology, 12. https://doi.org/10.3389/fmicb.2021.724449https://doi.org/10.3389/fmicb…
- Morin, C., Bokobza, C., Fleiss, B., Hill‑Yardin, E. L., Van Steenwinckel, J., & Gressens, P. (2023). Preterm birth by cesarean section: The gut‑brain axis, a key regulator of brain development. Developmental Neuroscience, 46(3), 179–187. https://doi.org/10.1159/000534124https://doi.org/10.1159/000534124
- Borrego‑Ruiz, A., & Borrego, J. J. (2024). Neurodevelopmental disorders associated with gut microbiome dysbiosis in children. Children, 11(7), 796. https://doi.org/10.3390/children11070796https://doi.org/10.3390/childre…


